Colonoscopy?
What is a Colonoscopy?
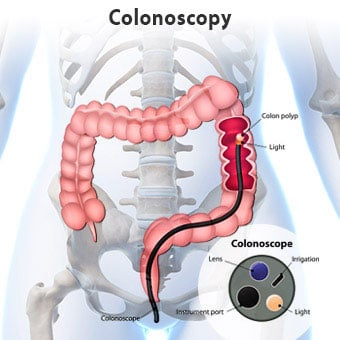
A colonoscopy is a test that allows your doctor to examine the lining of your colon for any abnormalities. The colonoscope, which is a thin,flexible, fiber optic instrument, is passed from your rectum to your cecum.
Colonoscopy is considered the “gold standard” to evaluate intestinal inflammation, ulceration, bleeding, diverticulosis and tumors. It is possible to remove most colon polyps during a colonoscopy, there is no pain or any sensation as the polyp is removed.
Do I have any alternatives for the test?
Depending on your symptoms and circumstances, it may bepossible to diagnose your bowel conditionusing a different test. Alternatives available are a Barium enema, CT scan, or, recently, virtual colonoscopy or a CT colonography. None of these tests see the textural details of the mucosal lining under magnification as does a colonoscopy. In your specific instance you may talk to your doctor about the relevance of these tests over a colonoscopy.
Are there any risks in the procedure?
Following colonoscopy, you may feel a little bloated for a short while. The commoner side effects of the
sedatives used include drowsiness, light-headedness and nausea. But the risk of a complication
happening during a diagnostic test is negligible(less than 0.01%). You to realize that you yourself can
minimize the risks when you read the following.
Being on blood thinning medications (Warfarin, clopidrogel, Xarelto, Eliquis, Aspirin, Naproxen) may
increase the risk of bleeding even from a simple biopsy during the colonoscopy. You may discuss this
with the endoscopist or your treating doctor. It is fine to take Acetaminophen or paracetamol.
You need to inform the endoscopy team in case you are already receiving the following medication, as
adequate precautions can be taken during the procedure:
- Diabetes medications such as Insulin or oral diabetes medications
- Heart problems or related surgeries, Heart valve replacement & Joint replacement;
Chemotherapy treatments or immunosuppressive drugs (steroids, azathioprine, etc) (you maythen need to have a prophylactic antibiotic during colonoscopy) - Kidney problems (to prevent drug side effects) Some
- medications such as for seizure disorders should not be stopped.
major Hospitals have stringent protocols for sterilization, and we assure that all aseptic - precautions are in place to prevent transmission of infections during Endoscopy.
What can be called the “Perfect Preparation” for a colonoscopy?
For your doctor to see the bowel wall clearly, the bowel needs to be completely empty. To help clear itout you will be asked to follow one of two protocols, if you want a fautless procedure The first involves drinking two liters of a solution of polyethylene glycol (Peglec or Colopeg) that causes temporary diarrhea. It comes in 2 flavors, which, unfortunately, only partially mask a somewhat unpleasant taste. Refrigerating the solution may make it more palatable. Drinking such a large volume of cold solution may cause a patient to feel chilled, but the sensation is temporary. Do not add flavoring (additional sugar or salt) to the solution. Many patients say that drinking the purgative solution is the most unpleasant part of the examination!
I usually prefer to ask patients to make the solution the night before; so they will not lose time making it when they wake up. You could drink it in two hours about 4 to 6 hours before the scheduled time for the test; at the rate of a glass (200 ml) every 10 minutes. In case you feel nauseous, slow down, so you do not throw up and need to start with a fresh two liter solution all over. You will pass about 5 to 8 watery stools, the last of which are expected to be the color of the solution you drank.
The second method involves drinking a solution called Exelyte (2 bottles of 45 ml each in a box) mixed in 300 ml lime juice or Limca over half an hour, followed by several glasses of fluids. This preparation is easier to consume (just 2 glasses of a juice, each over 15 minutes) than the Polyethylene glycol.
However, Exelyte is a cathartic; it makes you loose body water to make loose stools and you should be careful not to get dehydrated. I prefer to check that you do not already have a borderline renal damage (do a Blood urea & creatinine test); else giving this solution and not hydrating later may aggravate the kidney damage. It also contains a large amount of phosphorus, which may be a problem for people with heart or kidney conditions. It is very important that you drink frequently throughout the day to avoid dehydration. Drink water, soft drinks, fresh as well as canned juices, chicken or vegetable soups, coffee or tea (no milk; sugar is fine). Avoid foods with seeds the previous day (brinjal, guava) as well as supari & saunf; it remains undigested and then clogs our scopes!.
What to Wear
Please wear loose, comfortable clothing. Please leave your valuables at home. Wear comfortable, stable
shoes since you may be a little unsteady when you leave. You will be changing into a patient gown
before the procedure.
What actually happens in Colonoscopy?
With you resting on your left side, your doctor will gently examine your back passage with a gloved
finger & lubricating jelly before carefully inserting the colonoscope. Air is then usually passed through
the tube into the colon to make it expand and the bowel wall easier to see. This may briefly cause pains
similar to having wind and you may get an urge to go to the toilet, but as the colon is empty, this won’t
be possible.
Most people pass some wind. There is no need to feel embarrassed about this as your doctor will expect
this to happen. During the procedure, you may be asked to change your position – for example turning
from your side onto your back. This helps your doctor to examine different areas of the colon more
easily. If necessary, your doctor will take a biopsy and/or remove polyps. This is done using special
instruments passed inside the colonoscope, and is quick and painless.
I would prefer sedation for the procedure!
Our Anaesthesia team will make sure you are comfortable throughout the procedure. It would be
preferable for them to review your records in advance, so they can plan appropriately for the day of the
procedure. The sedative will be injected through the cannula placed in the back of your hand, and you
should start to feel relaxed and drowsy almost immediately. Sedatives can sometimes affect your
breathing, so the amount of oxygen in your blood will be monitored constantly through a clasp on your
finger and you may be given extra oxygen through a mask.
After your procedure is complete you will be taken to the recovery area. The nurses there will continue
to monitor your blood pressure, pulse and oxygen saturation. Your “significant other” or friend may
come sit with you in recovery at this time. You may need to stay in the recovery area for even up to
three hours. Plan so you do not need to drive, operate machinery, sign any important documents or
make important decisions until the next day. You should not exercise strenuously until the next day.
You must make arrangements for a responsible adult to drive you home after your procedure. Taxis and
buses are not permitted unless you are accompanied by a responsible adult.
