Neuroendocrine Tumors
What is a Neuroendocrine Tumors?
Neuroendocrine tumors are cancers that begin in specialized cells called neuroendocrine cells. Neuroendocrine cells have traits similar to those of nerve cells and hormone-producing cells.
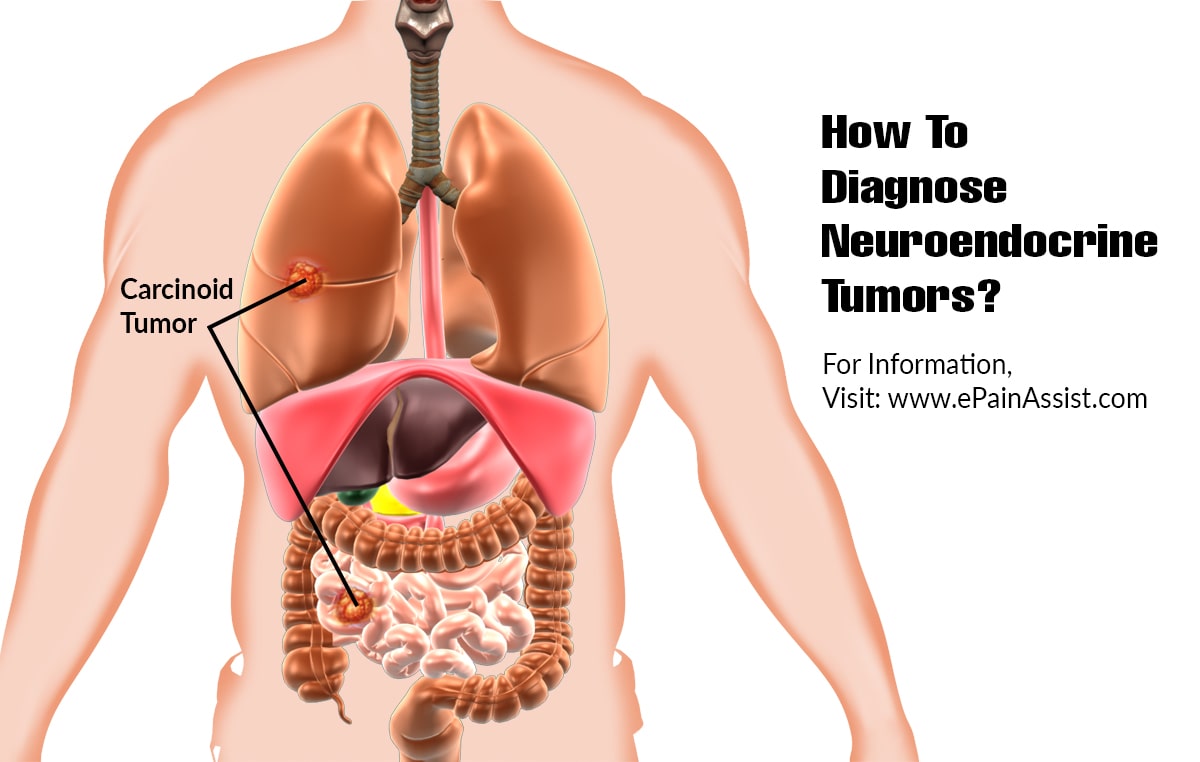
Neuroendocrine tumors are rare and can occur anywhere in the body. Most neuroendocrine tumors occur in the lungs, appendix, small intestine, rectum and pancreas.
There are many types of neuroendocrine tumors. Some grow slowly and some grow very quickly. Some neuroendocrine tumors produce excess hormones (functional neuroendocrine tumors). Others don’t release hormones or don’t release enough to cause symptoms (nonfunctional neuroendocrine tumors).
Symptoms
Neuroendocrine tumors don’t always cause signs and symptoms at first. The symptoms you might experience depend on the location of your tumor and whether it produces excess hormones.
In general, neuroendocrine tumor signs and symptoms might include:
- Pain from a growing tumor
- A growing lump you can feel under the skin
- Feeling unusually tired
- Losing weight without trying
Neuroendocrine tumors that produce excess hormones (functional tumors) might cause:
- Skin flushing
- Diarrhea
- Frequent urination
- Increased thirst
- Dizziness
- Shakiness
- Skin rash
Causes
The exact cause of neuroendocrine tumors isn’t known. These cancers begin in neuroendocrine cells that have traits similar to those of nerve cells and hormone-producing cells. Neuroendocrine cells are found throughout your body.
Neuroendocrine tumors begin when neuroendocrine cells develop changes (mutations) in their DNA. The DNA inside a cell contains the instructions that tell the cell what to do. The changes tell the neuroendocrine cells to multiply rapidly and form a tumor.
Some neuroendocrine tumors grow very slowly. Others are aggressive cancers that invade and destroy normal body tissue or spread (metastasize) to other parts of the body
Risk factors
The risk of neuroendocrine tumors is higher in people who inherit genetic syndromes that increase the risk of cancer. Examples include:
- Multiple endocrine neoplasia, type 1 (MEN 1)
- Multiple endocrine neoplasia, type 2 (MEN 2)
- Von Hippel-Lindau disease
- Tuberous sclerosis
- Neurofibromatosis
Treatments Neuroendocrine Tumors
Surgery
Removing the primary tumor with surgery is often the first approach recommended for patients with localized NETs. The goal of surgery is to fully remove a neuroendocrine tumor or reduce the tumor burden. Surgery may also be an option for those with advanced disease, to help relieve symptoms. Some surgical procedures for NETs include debulking or cytoreductive surgery, minimally invasive laparoscopic resections and liver transplantation.
Medical oncology
Depending on the type of NET and treatment goals, chemotherapy, hormone therapy and/or targeted therapy may be used to manage certain types of NETs, including advanced tumors. Some targeted therapies for pancreatic NETs include everolimus and sunitinib. Chemoembolization, in which chemotherapy drugs are administered directly into the tumor, may be an option if the disease has metastasized to the liver.
Radiation therapy
Radiation therapy is generally used when a neuroendocrine tumor has spread or is in a location that makes surgery difficult. CyberKnife® may be a non-invasive option for some patients and enables our radiation oncologists to deliver high, targeted doses of radiation to NETs. For metastatic disease to the liver, TheraSphere® and SIR-Spheres® offer innovative options that deliver radiation directly to tumors in the liver.
Interventional radiology
For NETs that have spread to the liver, embolization procedures may help reduce or cut off the supply of blood to the tumor.
Neuroendocrine Tumors
We provide a wide range of treatment options for gastrointestinal NETs. Our gastroenterology team uses various technologies to look at the GI tract in different and minimally invasive ways. We may recommend innovative techniques and ablative treatments to help remove obstructions in the GI tract and relieve pain or breathing problems.
Molecular targeted therapy
Peptide receptor radionuclide therapy (PRRT) is a molecular targeted therapy that may be used to treat certain NETs. Molecular targeted therapies use drugs or other substances to identify and attack cancer cells while reducing harm to healthy tissue.
